
ADVANCING HARM REDUCTION THROUGH THE LAW
The Issue
The United States is in the midst of a historic drug overdose and addiction crisis. Nationwide, the human, social, and economic costs associated with addiction, HIV transmission, and related issues are mounting. With the unfolding fiscal cliff in federal investments and scrambling of sensible public health policies, this situation is likely to worsen.
Fortunately, there are policies and programs to reduce these drug-related harms. Interventions include syringe service programs (SSPs), overdose education and naloxone distribution (OEND), drug checking services, 911 Good Samaritan laws (GSLs), and supervised consumption facilities (SCFs). Animated by the maxim of ‘meeting people where they’re at,’ harm reduction interventions equip and empower those who engage in risky substance use to make healthier choices. Harm reduction programs stand in contrast to punitive measures that have ballooned the prison population, increased overdoses and misdirected limited resources.
Despite a strong evidence base, harm reduction programs are tragically underutilized in the United States. Few states have authorized SSPs and a federal ban has not been fully lifted. This may also impact disbursement of federal funds for opioid crisis response, which are already scarce for SSPs and other harm reduction programs. Even after hard-won battles, progress has proved fragile in numerous jurisdictions.
Around the U.S., SSPs continue to face legal challenges, interference by law enforcement, and discriminatory regulation designed to suppress or extinguish operation. Many underground programs operate under constant threat of legal sanction and community opposition. Staff and client harassment and intimidation are not uncommon. Structural bottlenecks severely diminish the proven benefit of these programs to both clients and the community at large. When legal help is needed, there is often nowhere to turn; the harm reduction legal workforce is almost non-existent.
Legal and policy challenges also harm the behavioral health workforce. Recruitment and retention are chronically hampered by stress, burnout, and the perceived and real risk of legal liability.
Black and Brown communities, which have higher rates of overdose as well as incarceration for drug use, are disproportionately impacted, thereby exacerbating existing health disparities.
Our Response
The Advancing Harm Reduction through the Law (AHRLA) uses the law to protect harm reduction service providers and clients.
Community of Practice
Listserv
We convene legal professionals, advocates, and people with lived experience into a community of practice focused on advancing harm reduction through the law. This network facilitates rapid response, resource sharing, and strategy development across jurisdictions.
Are you a legal professional, advocate, or harm reduction worker interested in using the law to protect lifesaving services? Join our growing network.
Sign up for the Legal Advocates for Harm Reduction listserv to connect with others, receive updates on legal threats and strategies, and help build a stronger defense for harm reduction.
Convenings & Events
Panel discussion: National Strategies and Local Action in the Aftermath of Gather Church
A recent federal ruling in Gather Church v. Lewis County recognized harm reduction services as protected under the Americans with Disabilities Act, creating new opportunities to challenge discrimination.
Join national advocates, Connecticut leaders, and legal experts for a panel on the decision and its implications for harm reduction.
RSVP here for Zoom or in-person attendance.
Harm Reduction in the Headlines: Media Engagement 101
This interactive webinar examines how misinformation around harm reduction spreads and highlights practical strategies to safeguard your program
Using the Law to Protect Harm Reduction
We introduced our new legal toolkit designed to protect harm reduction programs. The session provides context on the legal landscape the toolkit responds to, the work behind its development, and opportunities for engagement as this work continues.
Post-Conference events Public Health Law Conference
We gathered in Renton, WA following the Network for Public Health Law Conference for two events, offered in collaboration with the Network for Public Health Law's Harm Reduction Legal Project.
-
Changing the Narrative on Harm Reduction: A half-day learning and strategy session on harm reduction and misinformation. Click here to learn more.
-
Legal Advocates for Harm Reduction Convening: The first in-person convening for the Legal Advocates for Harm Reduction. Click here to learn more.

Get
Legal
Help
HOTLINE:
We are developing a rapid response system for harm reduction programs and clients facing legal threats, such as program closures, law enforcement interference, and discriminatory policies. This system will match those affected with legal experts who can help.
Integrating Legal Navigation into Harm Reduction Programs:
COMING SOON!
Legal Practitioner Resources
We provide training and resources for law students, attorneys, and harm reduction workers. We are expanding the capacity of the legal field to support harm reduction. From the Americans with Disabilities Act to public health defenses, we are researching underused legal tools and deploying legal defense toolkits that can protect harm reduction services and challenge systemic discrimination. We help identify and support strategic legal action to establish legal precedent, expand protections, and amplify the voices of impacted communities.
About Us
Leo Beletsky - Director
Melissa Rothstein - Senior Legal Fellow
Arianna Murray - Legal Fellow
Sterling Johnson - Legal Fellow
Charlotte Lapsanksy - Changing the Narrative Lead
Andi Goodman - Pro-bono Advisor
Simon Kress - Pro-bono Advisor
Sunyou Kang - Director of Operations
Jule von der Heydt - Administrative Support
Interns
Christina Crowley
Ava Kominski
Aarti Sharma
Elizabeth Cronin
Evelyn Kung
Additional Information
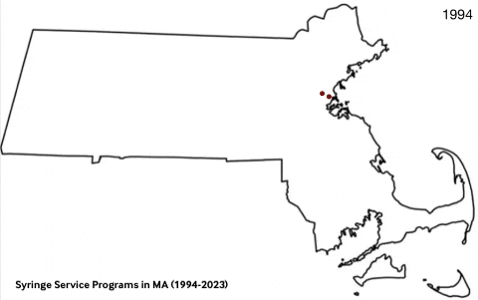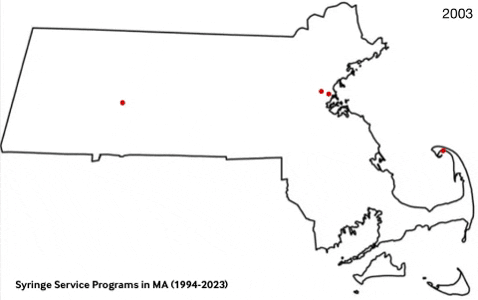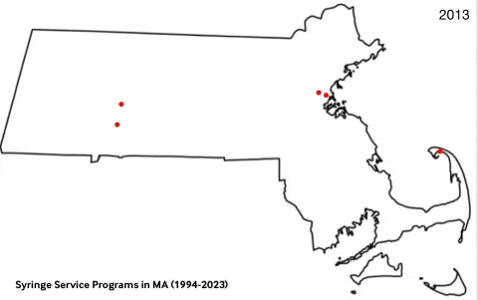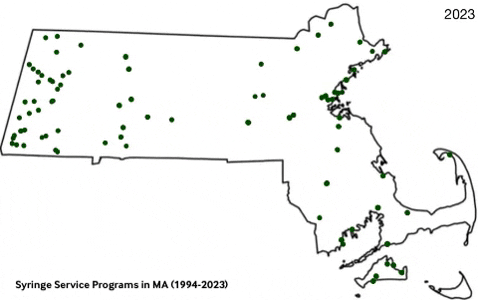
Data Dashboard
Massachusetts Syringe Exchange Programs (1994-2023)
Resources
Supervised Consumption Site
Opposition Response Paper & Advocacy Tool
Stigmatization of individuals experiencing substance use disorder (SUD) is pervasive in news media, medicine, and society. Supervised Consumption Sites (SCSs) are difficult to implement due to this stigmatization, despite considerable evidence showing that they prevent overdoses from turning fatal, increase safe injection hygiene, and improve access to SUD treatment. There are currently more than 100 sites in 11 countries achieving these outcomes. Multiple US cities are considering SCSs, however, none operate yet. This project assessed the landscape of SCS stigma in Boston to provide public health advocates the data necessary to respond to stigmatizations. First, we conducted a news and social media review in excess of 100 stories published by Boston news outlets between 2017-2020 about SCSs. We compiled negative public comments to identify SCS misconceptions in Boston. We found that Bostonians were concerned about increased crime, public spending, and condoning “illegal” activity. Second, these misconceptions were the basis for a comprehensive literature review on SCSs to aggregate considerable evidence responding to these misconceptions with evidence-based research. Ultimately, this culminated in an advocacy tool that is presently used in Boston’s harm reduction community.
This tool is designed for harm reduction advocates to counter misconceptions, community stigmas, and fears about supervised consumption sites with evidence-based research. This guide breaks down these myths and assumptions in an organized and aesthetic format that can be disseminated to educate the public.
Additionally, we produced a detailed research paper expanding on this analysis and the growing body of evidence in support of supervised consumption sites.
